By Aliza Rosen, a digital content strategist in the Office of External Affairs at the Johns Hopkins Bloomberg School of Public Health
A measles epidemic is currently escalating in the southwestern region of the United States, prompting public health officials to act swiftly to curb the spread and enhance vaccination efforts. Amid widespread misinformation regarding vaccines, health experts are increasingly alarmed that incidents like this may be on the rise.
This outbreak initiated in late January, and by February 25, Texas reported 124 confirmed cases—predominantly in Gaines County—with an additional nine cases in Lea County, New Mexico. A measles-related death reported on February 26 marks the first such fatality in the United States since 2015.
“The majority of the affected cases are traced back to a Mennonite community with a strong homeschool focus, which means they are exempt from school vaccination requirements,” notes Bill Moss, MD, MPH, a professor of Epidemiology and executive director of the International Vaccine Access Center.
In this question-and-answer session, he outlines essential information about measles, its transmission, and the critical importance of maintaining high vaccination rates to prevent future outbreaks.
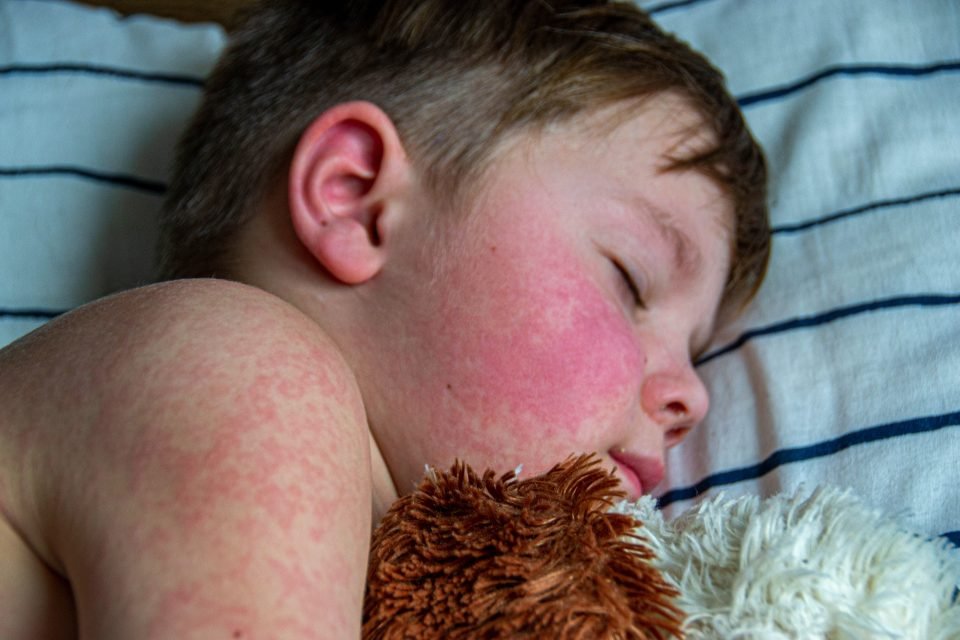
What is measles?
Measles is an extremely contagious illness caused by the measles virus. Symptoms typically include coughing, red eyes, a high fever, and a rash; however, it can also lead to severe health complications.
Is measles dangerous?
Yes, measles poses significant health risks. In the U.S., approximately 20% of unvaccinated individuals will require hospitalization due to measles. In 2024, this hospitalization rate was notably higher, with around 40% of those infected being hospitalized. Complications from measles can include pneumonia, encephalitis, brain damage, and complications during pregnancy. Importantly, these complications can affect anyone, including healthy adults and children.
Research has demonstrated that measles can erase the body’s memory of previous bacterial and viral infections, compromising the immune system and increasing susceptibility to other diseases, often lasting for years.
The disease can also have fatal outcomes; in 2023, approximately 107,500 individuals worldwide died from measles, primarily among unvaccinated or under-vaccinated children under five.
How does measles spread?
Measles transmission occurs through airborne particles and droplets. Infection can happen by inhaling air tainted by an infected individual or by touching a contaminated surface. The measles virus remains airborne for several hours after an infected person coughs or sneezes, signifying that close contact is not necessary for transmission.
Measles is among the most transmissible infectious diseases; in a population lacking immunity, one person with measles can infect, on average, 12 to 18 others.
Who is at the highest risk for contracting measles?
Individuals who haven’t received two doses of the measles, mumps, and rubella (MMR) vaccine or have never had measles are at high risk. In the U.S., this primarily includes children younger than 12 months who have yet to receive their initial MMR vaccine. There are also individuals who cannot be vaccinated due to medical conditions or severe allergies, including those who are immunocompromised or pregnant.
At what age should my child receive the MMR vaccine?
The CDC recommends the first dose of the MMR vaccine be given at 12 to 15 months of age, which protects approximately 93% to 95% of vaccinated children. The second dose is suggested at ages 4 to 6, typically before kindergarten, providing about 97% protection.
Can a child get the MMR vaccine earlier than 12 months old?
The MMR vaccine can be administered to children as young as 6 months. The CDC advises that when children aged 6 to 11 months are traveling internationally, they should receive the vaccine, although specific outbreak guidance in the U.S. is less clear. A dose given between 6 and 11 months is supplemental to the two recommended doses and not a substitute.
If you reside in or plan to travel to areas experiencing outbreaks, consult your pediatrician regarding whether your young child should receive an MMR dose earlier than the standard schedule. The CDC indicates that a second dose can be given earlier after at least 28 days from the first dose. Medical professionals can assist in evaluating local measles activity and vaccination levels.
If the measles vaccination is highly effective, why do I hear of continued measles cases?
The challenge lies in the fact that vaccination coverage is not universal. As measles is so highly contagious, it requires at least 95% of the population to be immunized to establish herd immunity. Currently, about 91% of children aged 19 to 35 months in the U.S. are vaccinated, yet coverage varies significantly in certain communities, elevating infection risk.
What factors have contributed to declining U.S. measles vaccination rates?
Several overlapping factors contribute to this decline, including the success of past immunization efforts. High vaccination rates historically have led to fewer measles cases, diminishing public concern about the illness and the perceived necessity for vaccination.
Parents aim to make the best choices for their children; however, with historically low incidence rates of measles and the widespread prevalence of misinformation surrounding vaccines, some parents may underestimate the dangers of measles while overestimating the risks associated with vaccinations.
How long after receiving the MMR vaccine does it take for protection to build?
It takes about two weeks for the body to develop antibodies after receiving the MMR vaccine, which are crucial for defending against future exposure.
If I had measles vaccinations in childhood, am I protected for life?
While most individuals vaccinated against measles enjoy lifelong protection—enhanced by receiving two doses—this immunity cannot be assumed for everyone. Those who respond positively to the vaccine are believed to remain protected indefinitely, with no evidence suggesting that immunity diminishes with age.
Adults vaccinated between 1963 and 1968 should verify their vaccination status, as a less effective inactivated version of the vaccine was used during that period, which was eventually withdrawn. Only a small fraction of today’s population received this outdated vaccine.
How can I determine if I’m immune to measles?
The best approach is to consult your vaccination records. If these are unavailable and you cannot recall your vaccination status, getting an additional measles vaccine dose is safe, even if you have previously been vaccinated or experienced natural immunity from an earlier infection.
Older adults born before 1957 are generally considered to have natural immunity due to previous exposure to the virus before vaccine development.
Blood tests available can assess antibodies against measles; these tests are particularly useful for immunocompromised individuals or those unable to receive the MMR vaccine. They are also routinely conducted to ensure healthcare workers are adequately protected, especially those in pediatric or high-exposure environments.
Is it safer for children to contract measles naturally rather than receive the vaccine?
No. Measles is a hazardous disease, while the vaccine is very safe. The potential dangers of severe illness, complications, or even death associated with measles far exceed the mild side effects some may experience after vaccination. Serious adverse reactions to the MMR vaccine are rare.
Where can I obtain a measles vaccination?
Measles vaccinations are generally available at medical offices, clinics, and public health centers. During outbreaks, local health departments may offer MMR vaccination clinics to enhance community protection. For information, check with your local or state health department.
How can I stay informed about measles activity in my area?
The CDC website is an excellent resource for monitoring national outbreak trends. State health departments, which report to the CDC, also provide valuable information. In states experiencing outbreaks, local and state health departments may share more frequent updates to inform communities about ongoing incidents and recommended safety measures.
Measles is among the most contagious diseases, yet it is also preventable through vaccination.
Where can I find more information about measles?
For comprehensive details, visit the CDC’s pages on measles and vaccination. The WHO also provides globally relevant information regarding measles and its consequences through its fact sheet.
Article authored by Aliza Rosen, a digital content strategist in the Office of External Affairs at the Johns Hopkins Bloomberg School of Public Health.
Copyright for this text is held by The Johns Hopkins University. This article is reproduced for educational purposes with the permission of the Johns Hopkins Bloomberg School of Public Health, Baltimore, MD.
For all other usage, written permission is required.
Editor’s Note: The content provided here is not intended to replace professional medical advice, diagnosis, or treatment, and does not constitute medical or professional advice.





